The global pandemic of COVID-19 has already had a significant impact on the health care system and on cardiac services, even outside of epicenters and major cities like New York. Perhaps one of the most pressing issues for clinicians is the exceedingly practical consideration of wearing suddenly scarce personal protective equipment like surgical masks. It is a question critical to quality care as we navigate these difficult times, so we’ve gathered a diverse array of perspectives to offer some insight. COVID-19 and cardiology are also intrinsically linked, with the disease’s impact on cardiac injury being scrutinized more closely. This edition of Quality Matters hopefully summarizes priorities of what you need to know, right now.

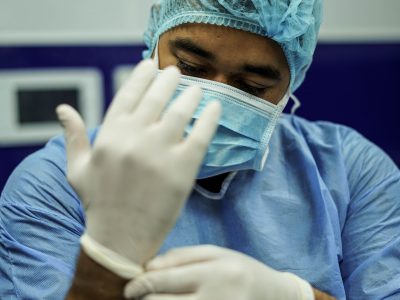
To mask, or not to mask?
Unfortunately, it’s not so straightforward a question. Practical realities like shortages in personal protective equipment are forcing clinicians to ask this question of their organizations and make difficult policy decisions. Here’s some insight into the problem, and potentially helpful resources:
Mixed Messages on COVID-19 Masks: Science Falls Short As Deaths Mount – TCTMD
An excellent feature by Shelley Wood of TCTMD takes a look at clinician’s perspectives on both sides of the issue, as well as the “shaky evidence base” guiding decision-making on either side. “Workers in other hard-hit countries are taking pains to explain the personal protective measures they’ve taken, including ubiquitous use of masks in countries where the outbreak appears to have turned a corner,” writes Wood for TCTMD. “A minority of US hospitals are following suit.”
Other hospitals and clinicians are taking the stance that they’d quickly burn through supply if all health care workers were required to wear masks. A spokesperson for Banner Health in Arizona told TCTMD that “Banner does not endorse personal mask use as effective in preventing disease transmission.” Especially considering the “right way” to use a mask—disposing of it after every patient encounter. “By having to use it for a day or multiple days, the bad thing is we may be turning the doctor into a viral vector if they are wandering around among people who do not have the infection,” said C. Michael Gibson, MD.
“If only we in the USA had enough PPE. Compare this to universal mask policies in which staff are given one surgical mask per shift.#COVID19 Make no mistake, I don’t have the answer, but wonder about real protection vs facades of protection,” said John Mandrola, MD on Twitter.
‘Stealth Transmission’ of COVID-19 Demands Widespread Mask Usage – Medscape Commentary
A commentary written by Eldad Einav, MD a cardiologist at Our Lady of Lourdes Memorial Hospital in Binghamton, New York takes a firm stance in favor of universal mask policies. “To be clear, mask use is one of the most effective physical interventions to prevent the spread of respiratory viruses. A comprehensive Cochrane review examined multiple physical preventive measures (eg, screening at entry ports, isolation, quarantine, social distancing, barriers, personal protection, hand hygiene) and found that masks were the most consistent and comprehensive measure,” he writes. “So why not recommend universal usage, for HCWs and the community alike? The main reason given by authorities is that there is no evidence showing that it is effective in the community. However, “there is an essential distinction between absence of evidence and evidence of absence,” write Hong Kong scholars in a comment in The Lancet . The paucity of data regarding widespread mask use does not mean that masks are not effective.” He continues to argue that mounting evidence of asymptomatic shedding of the disease, or ‘stealth transmission’ demands widespread mask usage. Read more »
Fair Allocation of Scarce Medical Resources in the Time of Covid-19 – New England Journal of Medicine
Perhaps a seminal article in this discussion is this article released March 23 in the New England Journal of Medicine, regarding how best to steward and ration critical resources like ventilators and personal protective equipment. “Because maximizing benefits is paramount in a pandemic, we believe that removing a patient from a ventilator or an ICU bed to provide it to others in need is also justifiable and that patients should be made aware of this possibility at admission,” write the authors. “Critical Covid-19 interventions — testing, PPE, ICU beds, ventilators, therapeutics, and vaccines — should go first to front-line health care workers and others who care for ill patients and who keep critical infrastructure operating, particularly workers who face a high risk of infection and whose training makes them difficult to replace. These workers should be given priority not because they are somehow more worthy, but because of their instrumental value: they are essential to pandemic response.”
And perhaps most practical in their recommendations is how organizations might institute their recommendations in practice: “To help clinicians navigate these challenges, institutions may employ triage officers, physicians in roles outside direct patient care, or committees of experienced physicians and ethicists, to help apply guidelines, to assist with rationing decisions, or to make and implement choices outright — relieving the individual front-line clinicians of that burden,” write the authors. Read more »

Care Questions: COVID-19 and Cardiology
Of course, you also need to know the latest on how COVID-19 and cardiology interact, how the disease is affecting patients with cardiovascular disease, and the potential link between COVID-19 and cardiac injury. Here are the latest guidelines and insight:
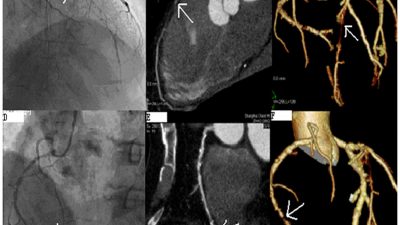
Cardiac injury among hospitalized Covid-19 patients tied to higher risk of death in new study – CNN Health
It may be important to note that a new study published March 25 associating cardiac injury with mortality in hospitalized patients with COVID-19 has received widespread media attention in and out of cardiology-specific news sources. “The data also revealed that the death rate was higher among patients with cardiac injury versus those without: 42 of the patients with cardiac injury, or 51.2%, died versus 15 of those without, or 4.5%,” summarizes CNN Health. “In addition, preexisting cardiovascular diseases might also be more susceptible COVID-19–induced heart injury, as approximately 30% and 60% of patients with cardiac injury in the present study had a history of coronary heart disease and hypertension, respectively, which were significantly more prevalent than in those without cardiac injury,” wrote the study’s authors. Read more »
CSC Expert Consensus on Principles of Clinical Management of Patients with Severe Emergent Cardiovascular Diseases during the COVID-19 Epidemic – Circulation
The English translation of this expert consensus document from the Chinese Society of Cardiology was published March 27 in Circulation from the American Heart Association, providing insight into how invasive cardiologists in China are managing emergent cases. The document covers recommendations for triage for emergent cases as well as recommending principles for treatment and COVID-19-specific strategies when intervention is necessary. Read the full text »