Outcomes-focused research made news across cardiology disciplines in the past few weeks, highlighting cardiology services impacting outcomes. One study points out the potential impact of taking cardiac rehabilitation “to the next level,” as individualized rehab provides an opportunity for service lines to improve outcomes across the board. Plus, a large qualitative study offers insight into top-performers in responding to in-hospital cardiac arrest.
Also, a new consensus document on PCI for chronic total occlusion offers a path forward for improving quality and consistency in the procedure world-wide, and contradictory landmark studies offer insight into management of acute hypertension in individuals with intracerebral hemorrhage.

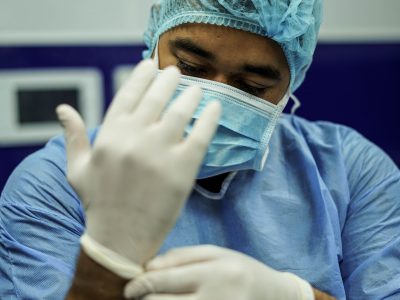
Cardiac Rehab Provides Opportunity to Improve Outcomes After CV Events – Healio Cardiology
“Cardiac rehabilitation has been neglected,” argues Pam R. Taub, MD, FACC, director of the Step Family Cardiac Wellness Rehabilitation Center and associate professor of medicine at UC San Diego in a presentation at the American Society for Preventive Cardiology Congress on CVD Prevention. “More and more hospitals are realizing that it’s a service line and that we all have to work together… because working together yields improved outcomes.”
Reimbursement for cardiac rehabilitation is on the rise thanks to value-based care initiatives, and new technology like wearables offer opportunities for clinicians to be more innovative and individualized to have maximum impact on CV outcomes. But despite the clear benefit and further potential of cardiac rehabilitation programs, many physicians are not recommending it, says Taub. “When we make that recommendation, [patients are] much more likely to follow it.” Read more »
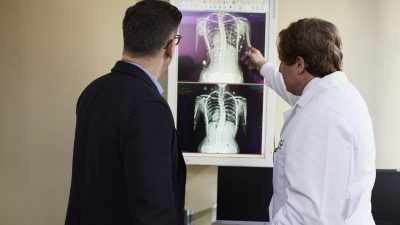
Dedicated Cardiac Arrest Rapid Response Teams Get Best Results – Medscape
Findings published recently in JAMA Internal Medicine showed, perhaps unsurprisingly, that dedicated rapid response teams with “little to no other competing clinical responsibilities” were top-performing in terms of in-hospital cardiac arrest survival. The large qualitative study provides significant insight into improving procedures and outcomes surrounding in-hospital cardiac arrest. “We also found several patterns where rapid response teams collaborated quite closely with bedside nurses, not just during a rapid response, but actually also in anticipation of a rapid response,” said author Saket Girotra, MD, SM of the University of Iowa to Medscape. “The bedside nurses felt trusted and empowered to call for a rapid response.” Read more »
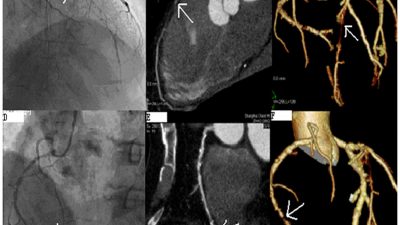
CTO PCI Consensus Document Aims for Quality, Consistency but Acknowledges Data Gaps – TCTMD Heart Beat
“The field has matured significantly, and for people who want to start doing this, these are some of the key concepts that you have to adhere to to have the best outcomes in CTO interventions,” says lead author Emmanouil Brilakis, MD, PhD of the Minneapolis Heart Institute to TCTMD. The paper, released in the most recent issue of Circulation, outlines seven key principles for CTO PCI practice—notably, that ischemic symptom improvement is the primary indication. Eric Bates, MD, of the University of Michigan offered TCTMD the third-party insight that the document was “honest and measured” in stating up-front that CTO PCI “is primarily indicated for symptom and not outcome improvement at this time.” The paper acknowledges the lack of randomized trial data proving the procedure can reduce negative outcomes. Read more »
BP Variability After Intracerebral Hemorrhage Linked to Poor Clinical Outcomes – Cardiology Advisor
In a recent editorial published in Stroke, Alejandro A Rabinstein, MD, Professor of Neurology at Mayo Clinic, synthesized contradictory results regarding management of acute hypertension in individuals with intracerebral hemorrhage (ICH) from two major controlled landmark trials. “He believes focusing exclusively on blood pressure targets may obscure a critical finding, specifically, the potential link between fluctuations in BP during the hyperacute phase and poor outcomes for individuals with ICH,” reads the article in Cardiology Advisor. “BP fluctuations portend poor outcome and suggest that avoiding these fluctuations could represent a valid therapeutic target,” says Rabinstein. Read more »